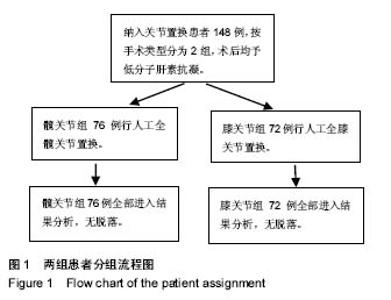
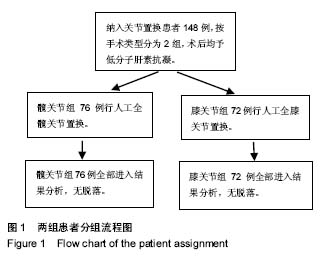
Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (3): 329-335.doi: 10.3969/j.issn.2095-4344.0026
Association of thrombelastogram with postoperative hemorrhage after total joint arthroplasty by structural equation modeling
Zhang Ying-bin1, Xu Jie1, Weng Jian-hao1, 2, Li Deng1, Cai Zhi-qing1, Huang Yu-lin1, Su Bao-hua1, Ma Ruo-fan1
- 1Department of Joint Surgery, Sun Yat-sen Memorial Hospital, Sun Yat-sen University, Guangzhou 510120, Guangdong Province, China; 2Grade of 2013, 8-year Program of Clinical Medicine, Sun Yat-sen University, Guangzhou 510275, Guangdong Province, China
-
Online:2018-01-28Published:2018-01-28 -
Contact:Ma Ruo-fan, Master, Chief physician, Department of Joint Surgery, Sun Yat-sen Memorial Hospital, Sun Yat-sen University, Guangzhou 510120, Guangdong Province, China -
About author:Zhang Ying-bin, Studying for master’s degree, Department of Joint Surgery, Sun Yat-sen Memorial Hospital, Sun Yat-sen University, Guangzhou 510120, Guangdong Province, China -
Supported by:the Science and Technology Program of Guangdong Province, No. 2014A020215009
CLC Number:
Cite this article
Zhang Ying-bin, Xu Jie, Weng Jian-hao, Li Deng, Cai Zhi-qing, Huang Yu-lin, Su Bao-hua, Ma Ruo-fan. Association of thrombelastogram with postoperative hemorrhage after total joint arthroplasty by structural equation modeling [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(3): 329-335.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
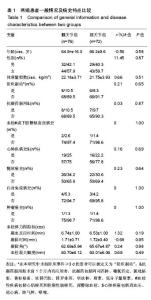

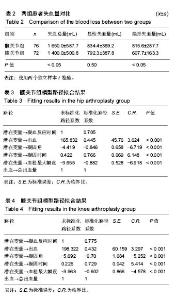
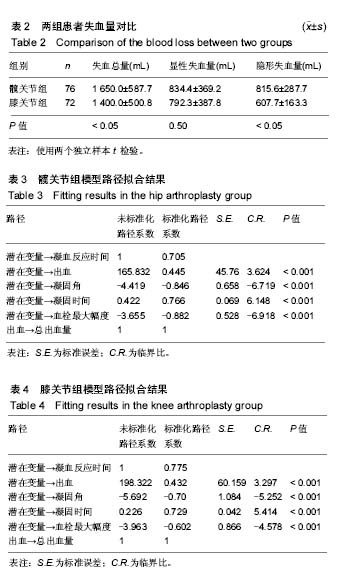
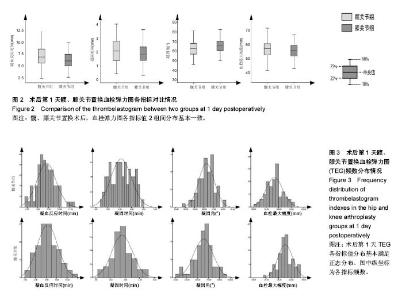
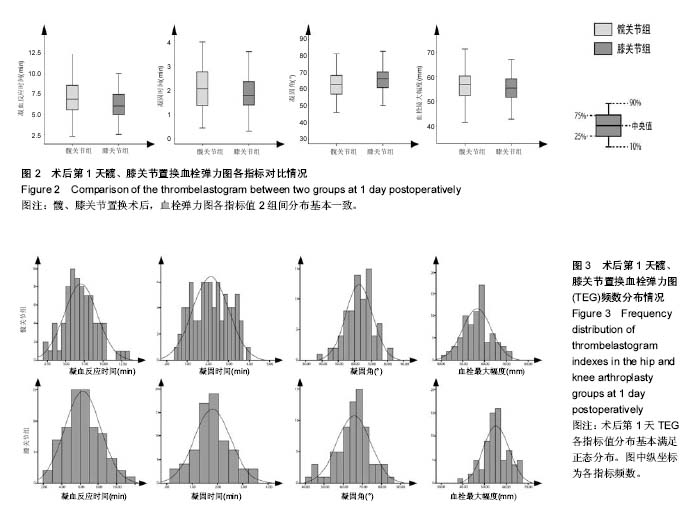
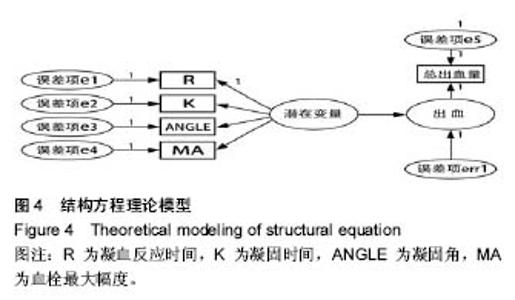
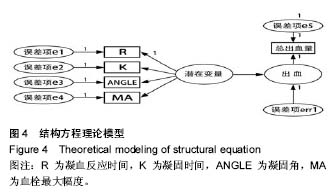
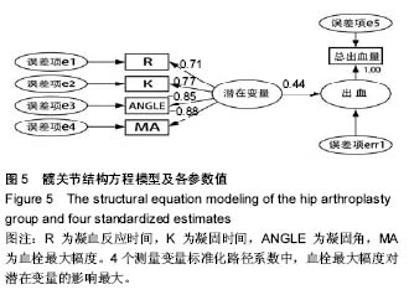
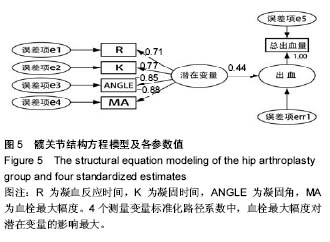
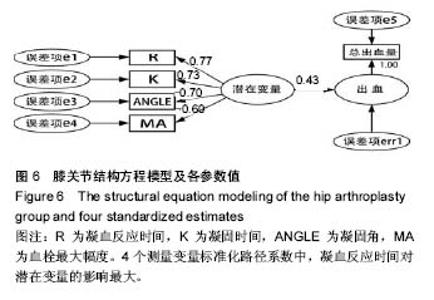
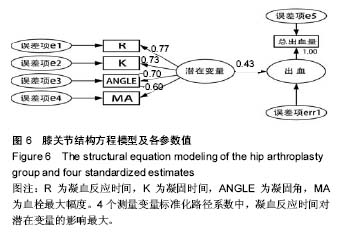
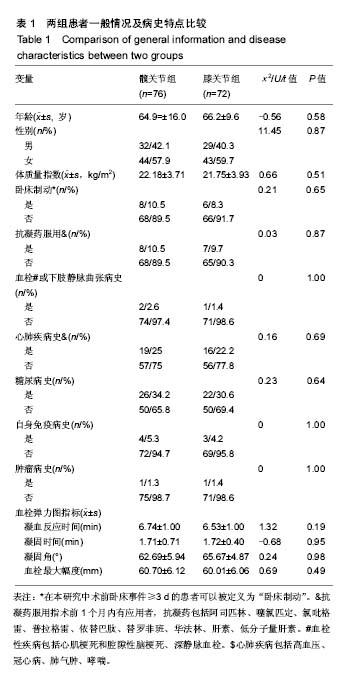
2.2 基线水平及出血情况 本研究髋、膝关节置换者2组病例一般情况见表1。2组间关于年龄、体质量指数和凝血指标等计量资料的区别通过Mann-Whitney U 检验、独立样本t 检验建议进行比较;对性别、卧床制动情况、药物和疾病史等计数资料通过卡方检验比较。如表1所示,组间就年龄、卧床制动情况、心肺病史方面差异无显著性意义。术前TEG所属4个指标差异无显著性意义。 统计髋、膝关节置换者2组病例术后均未予输血、补铁、促红细胞生成素等措施纠正贫血措施,术后失血总量、显性失血量及隐形失血量(见表2),虽失血量有差异,但其百分比构成较为接近。2组患者失血总量、隐性出血量间的差异有显著性意义(P < 0.05),而显性出血量2组间差异无显著性意义(P=0.50)。 2.3 术后第1天TEG 术后第1天所有入组患者均复测TEG,记录凝血反应时间、凝固时间、凝固角、血栓最大幅度值。术后第1天TEG 4个指数分布情况如图2,3所示,术后第1天患者凝血反应时间、凝固时间较正常值缩短,凝固角、血栓最大幅度稍增大。 2.4 结构方程模型 凝血反应时间、凝固时间、凝固角、血栓最大幅度4个观察值与总出血量之间的关系,使用结构方程模型进行分析,由于凝血反应时间、凝固时间、凝固角、血栓最大幅度4个观察变量存在相关性,故用构建潜在变量(indicator)的来消除观察变量的相关性,潜在变量可以避免重复抽取观察变量中相同的信息,仅抽取各观察变量中有差异的信息,保证了信息不会重复。根据理论研究,外因潜在变量Indicator为显性变量,其有凝血反应时间、凝固时间、凝固角、血栓最大幅度等4个测量变量,内因潜在变量(出血)为显性变量,观察变量为总出血量。潜在变量Indicator对内因潜在变量(出血)有直接的影响。E1-e5分别为观察变量凝血反应时间、凝固时间、凝固角、血栓最大幅度与总出血量的误差项,err1为内因潜在变量的误差项。因为内因潜在变量(出血)只有一个观察变量,需将观察变量总出血量的误差项的方差固定为1,且同时认为观察变量总出血量可以完全反映总出血量的特质,故将总出血量到总出血量的路径系数固定为1,见图4。 构建结构方程理论模型后,分别纳入髋、膝关节置换术后第1天TEG 4个变量与总出血量进入理论模型并进行拟合并研究凝血反应时间、凝固时间、凝固角、血栓最大幅度4个观察值与总出血量之间的关系。由表3可见,髋关节置换组潜在变量与4个观察变量标准化回归系数水平分别为:凝血反应时间=1.00(P < 0.05),凝固时间=0.766(P < 0.05),凝固角=-0.846(P < 0.05),血栓最大幅度=-0.882(P < 0.05)。indicator和凝血反应时间、凝固时间、凝固角、血栓最大幅度4个值之间存在相关性。模型拟合结果绝对适配指数近似误差均方根为0.044小于0.08,拟合优度指数与调整拟合优度指数值均高于0.9;增值适配指数规范拟合指数值与比较拟合指数值均高于0.9;简约适配度指数χ2/df为1.540小于2。绝对适配指数、增值适配指数、简约适配度指数符合标准,理论模型与数据匹配的(见图5)。indicator与总出血量之间也存在相关性(标准化回归系数=0.445,CR=3.624,P < 0.05)。而由表4可见,膝关节置换组潜在变量indicator和凝血反应时间、凝固时间、凝固角、血栓最大幅度4个值之间也存在相关性。模型拟合结果绝对适配指数近似误差均方根为0.017小于0.08,拟合优度指数与调整拟合优度指数值均高于0.9;增值适配指数规范拟合指数值与比较拟合指数值均高于0.9;简约适配度指数χ2/df为1.540小于2。绝对适配指数、增值适配指数、简约适配度指数符合标准,理论模型与数据匹配(见图6)。indicator与总出血量之间也存在相关性(标准化回归系数=0.432,CR=3.297,P < 0.05)。 "
| [1] Jauregui JJ, Boylan MR, Kapadia BH, et al. Total joint arthroplasty in nonagenarians: what are the risks? J Arthroplasty. 2015;30(12): 2102-2105.[2] Springer BD, Beaver WB, Griffin WL, et al. Role of surgical dressings in total joint arthroplasty: a randomized controlled trial. Am J Orthop (Belle Mead NJ). 2015;44(9):415-420.[3] Halawi MJ. Outcome measures in total joint arthroplasty: current status, challenges, and future directions. Orthopedics. 2015;38(8): e685-e689.[4] Daines BK, Dennis DA, Amann S. Infection prevention in total knee arthroplasty. J Am Acad Orthop Surg. 2015;23(6):356-364.[5] Aumiller WD, Kleuser TM. Recognizing and managing infections in total joint arthroplasty. JAAPA. 2015;28(6):37-41.[6] Gaspar MP, Kane PM, Shin EK. Management of complications of wrist arthroplasty and wrist fusion. Hand Clin. 2015;31(2):277-292.[7] Yu S, Garvin KL, Healy WL, et al. Preventing hospital readmissions and limiting the complications associated with total joint arthroplasty. J Am Acad Orthop Surg. 2015;23(11):e60-e71.[8] Takedani H, Ohnuma K, Hirose J. Deep venous thrombosis was not detected after total knee arthroplasty in Japanese patients with haemophilia. Haemophilia. 2015;21(5):585-588.[9] An TJ, Engstrom SM, Oelsner WK, et al. Elevated d-Dimer is not predictive of symptomatic deep venous thrombosis after total joint arthroplasty. J Arthroplasty. 2016;31(10):2269-2272.[10] Kim YH, Kulkarni SS, Park JW, et al. Prevalence of deep vein thrombosis and pulmonary embolism treated with mechanical compression device after total knee arthroplasty in Asian patients. J Arthroplasty. 2015;30(9):1633-1637.[11] Westrich GH, Haas SB, Mosca P, et al. Meta-analysis of thromboembolic prophylaxis after total knee arthroplasty. J Bone Joint Surg Br. 2000;82(6):795-800.[12] Imperiale TF, Speroff T. A meta-analysis of methods to prevent venous thromboembolism following total hip replacement. JAMA.1994;271 (22):1780-1785.[13] Gillespie W, Murray D, Gregg PJ, et al. Risks and benefits of prophylaxis against venous thromboembolism in orthopaedic surgery. J Bone Joint Surg Br. 2000;82(4):475-479.[14] Clarke MT, Green JS, Harper WM, et al. Screening for deep-venous thrombosis after hip and knee replacement without prophylaxis. J Bone Joint Surg Br.1997;79(5):787-791.[15] 邱贵兴. 中国骨科大手术静脉血栓栓塞症预防指南[J]. 中华关节外科杂志(电子版), 2009,3(3):380-383.[16] Bell TH, Berta D, Ralley F, et al. Factors affecting perioperative blood loss and transfusion rates in primary total joint arthroplasty: a prospective analysis of 1642 patients. Can J Surg. 2009;52(4):295-301.[17] Raskob GE, Hirsh J. Controversies in timing of the first dose of anticoagulant prophylaxis against venous thromboembolism after major orthopedic surgery.. Chest. 2003;124(6):379S-385S.[18] 许杰,马若凡,李登,等. 肝硬化患者人工全髋关节置换围手术期深静脉血栓形成风险及个体化抗凝治疗的研究[J]. 中华骨科杂志, 2015,35(11): 1096-1104.[19] 许杰,黄晶,马若凡,等.人工髋关节置换肝硬化患者围置换期的处理[J]. 中国组织工程研究, 2013,17(52):8967-8973.[20] van Helmond N, Johnson BD, Curry TB, et al. Coagulation changes during lower body negative pressure and blood loss in humans. Am J Physiol Heart Circ Physiol. 2015;309(9):H1591-H1597.[21] Chapin JC, Hajjar KA. Fibrinolysis and the control of blood coagulation. Blood Rev. 2015;29(1):17-24.[22] Eckman MH, Erban JK, Singh SK, et al. Screening for the risk for bleeding or thrombosis. Ann Intern Med. 2003;138(3):W15-W24.[23] Mallett SV, Cox DJ. Thrombelastography. Br J Anaesth. 1992;69(3): 307-313.[24] Hartert H. Blutgerinnungsstudien mit der Thrombelastographie, einem neuen Untersuchungsverfahren. Klinische Wochenschrift. 1948;26(37): 577-583.[25] Pfanner G, Koscielny J, Pernerstorfer T, et al. Preoperative evaluation of the bleeding history. Recommendations of the working group on perioperative coagulation of the Austrian Society for Anaesthesia, Resuscitation and Intensive Care. Anaesthesist.2007;56(6): 604-611.[26] Spiess BD, Gillies BS, Chandler W, et al. Changes in transfusion therapy and reexploration rate after institution of a blood management program in cardiac surgical patients. J Cardiothorac Vasc Anesth. 1995;9(2):168-173.[27] Luddington RJ. Thrombelastography/thromboelastometry. Clin Lab Haematol. 2005;27(2):81-90.[28] Esnault P, Prunet B, Cungi PJ, et al. Thromboelastometric profile of unwashed shed blood after primary knee arthroplasty. Transfus Clin Biol. 2015;22(1):30-36.[29] Na HS, Shin HJ, Lee YJ, et al. The effect of tranexamic acid on blood coagulation in total hip replacement arthroplasty: rotational thromboelastographic(ROTEM(R)) analysis. Anaesthesia. 2016;71(1): 67-75.[30] Elliott A, Wetzel J, Roper T, et al. Thromboelastography in patients with acute ischemic stroke. Int J Stroke. 2015;10(2):194-201.[31] Kane I, Ong A, Orozco FR, et al. Thromboelastography predictive of death in trauma patients. Orthop Surg. 2015;7(1):26-30.[32] Tekkesin N, Tekkesin M, Kaso G. Thromboelastography for the monitoring of the antithrombotic effect of low-molecular-weight heparin after major orthopedic surgery. Anatol J Cardiol. 2015;15(11):932-937.[33] Ward CF, Meathe EA, Benumof JL, et al. A computer nomogram for blood loss replacement. Anesthesiology. 1980;53(3):S126.[34] Nadler SB, Hidalgo JH, Bloch T. Prediction of blood volume in normal human adults. Surgery. 1962;51(2):224-232.[35] Hong E, Kang YS. Structural equation modeling on healthy menopausal transition. J Korean Acad Nurs. 2015;45(1):64-75.[36] Jacobucci R, Grimm KJ, McArdle JJ. Regularized structural equation modeling. Struct Equ Modeling. 2016;23(4):555-566.[37] Hasman A. An introduction to structural equation modeling. Stud Health Technol Inform. 2015;213:3-6.[38] Cook MR, Louis SG, McCully SP, et al. Positive blood alcohol is associated with reduced DVT in trauma. Injury. 2015;46(1):131-135.[39] Connelly CR, Yonge JD, McCully SP, et al. Assessment of three point-of-care platelet function assays in adult trauma patients. J Surg Res. 2017;212:260-269.[40] Connelly CR, Van PY, Hart KD, et al. Thrombelastography-based dosing of enoxaparin for thromboprophylaxis in trauma and surgical patients: A Randomized Clinical Trial. JAMA Surg. 2016;151(10):e162069.[41] Konig G, Yazer MH, Waters JH. The effect of salvaged blood on coagulation function as measured by thromboelastography. Transfusion. 2013;53(6):1235-1239.[42] Kashuk JL, Moore EE, Wohlauer M, et al. Initial experiences with point-of-care rapid thrombelastography for management of life-threatening postinjury coagulopathy. Transfusion. 2011;52(1):23-33.[43] Klein SM, Slaughter TF, Vail PT, et al. Thromboelastography as a perioperative measure of anticoagulation resulting from low molecular weight heparin: a comparison with anti-Xa concentrations. Anesth Analg. 2000;91(5):1091-1095.[44] Yang Y, Yao Z, Dai W, et al. Changes of thrombelastography in patients undergoing elective primary total knee and total hip replacement with low molecular heparin prophylaxis. J Orthop Surg Res. 2014;9:52.[45] Holcomb JB, Minei KM, Scerbo ML, et al. Admission rapid thrombelastography can replace conventional coagulation tests in the emergency department: experience with 1974 consecutive trauma patients. Ann Surg. 2012;256(3):476-486.[46] Wilson D, Cooke EA, McNally MA, et al. Changes in coagulability as measured by thrombelastography following surgery for proximal femoral fracture. Injury. 2001;32(10):765-770.[47] Vig S, Chitolie A, Bevan DH, et al. Thromboelastography: a reliable test? Blood Coagul Fibrinolysis. 2001;12(7):555-561.[48] Dickinson KJ, Troxler M, Homer-Vanniasinkam S. The surgical application of point-of-care haemostasis and platelet function testing. Br J Surg. 2008;95(11):1317-1330.[49] Mccrath DJ, Cerboni E, Frumento RJ, et al. Thromboelastography maximum amplitude predicts postoperative thrombotic complications including myocardial infarction.. Anesthesia Analgesia. 2005;100(6): 1576-1583.[50] Bai J, Zheng QW, Fu SH, et al. Association between thrombelastography system and thromboembolic and bleeding events in Chinese aged people. Int J Clin Exp Med. 2013;6(4):310-319. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [3] | Li Dadi, Zhu Liang, Zheng Li, Zhao Fengchao. Correlation of total knee arthroplasty efficacy with satisfaction and personality characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1346-1350. |
| [4] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [5] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [6] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [7] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [8] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [9] | Yuan Jiawei, Zhang Haitao, Jie Ke, Cao Houran, Zeng Yirong. Underlying targets and mechanism of Taohong Siwu Decoction in prosthetic joint infection on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1428-1433. |
| [10] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [11] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [12] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [13] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Influence of anterior cruciate ligament defect on the mid-term outcome of fixed-bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 860-865. |
| [14] | Zhang Nianjun, Chen Ru. Analgesic effect of cocktail therapy combined with femoral nerve block on total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 866-872. |
| [15] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||